Get back to the activities you love, without surgery.
Receive a Regenexx® Patient Info Packet by email to learn more about our regenerative orthopedic procedures.Regenexx® Non-Surgical Procedures for Spine-Related Conditions.
The board-certified, highly skilled physicians who are part of the Regenexx Network have a range of regenerative orthopedic procedures developed to help reduce pain, improve function and avoid spine surgery and the damaging side effects of epidural steroid injections. These highly specific, precise image-guided injection procedures use the healing agents from your own body to promote the body’s natural healing ability in treating bulging or herniated discs, degenerative conditions in the spine, and other back and neck conditions.
The origin of spine pain is often misidentified which can lead to inappropriate treatment and unnecessary surgery. Being the pioneers of the field of Interventional Orthobiologics, and more than a decade and a half of experience in using these advanced Interventional Orthobiologics procedures for spine pain, our highly-skilled board-certified physicians are able to identify the most probable sources of pain and select the most appropriate non-surgical minimally-invasive treatment options available.
Commonly Treated Spine / Cervical Conditions
This is not a complete list of conditions treated and some of these conditions may not be treated by our doctors, so please contact us or complete the Regenexx Candidate Form if you have questions about whether you or your condition can be treated with these non-surgical procedures.
- Annular Tear
- Arthritis of the Spine
- Back Pain
- Bone Spurs
- Bulging Disc
- Canal Stenosis
- Collapsed Disc
- Degenerative Disc Disease
- Degenerative Spine
- Disc Extrusion / Protrusion
- Facet Joint Syndrome
- Failed Back Surgery Syndrome
- Foraminal Stenosis
- Herniated Disc
- Herniated Nucleus Pulposus (HNP)
- Neck Pain
- Nerve Pain
- Pinched Nerves
- Radiculitis
- Radiating Nerve Pain
- Ruptured Disc
- Sciatica
- SI Joint Syndrome
- Slipped Disc
- Spinal Stenosis
- Spondylosis
- Torn Disc
- Radiculopathy
Patient Outcome Data
About Regenexx and our Hightly Skilled Physician Network
Regenexx Physicians represent a very selective, highly-skilled, interventional orthopedics network that is 100% focused on orthopedic conditions. All Regenexx physicians are musculoskeletal experts with extensive training and experience in the diagnosis and treatment of musculoskeletal conditions, as well as complex, image-guided injections of your body’s own healing agents to treat orthopedic issues. Regenexx patient outcomes are tracked in a registry and with that information, we provide transparent outcome data (below) for those who may be considering this treatment option.
Regenexx Lumbar Spine/Back Webinar
Learn About Regenexx Regenerative Orthopedic Procedures for Back/Spine Injuries.
View WebinarRegenexx Lumbar Spine/Back Webinar
Regenexx Alternative to Spine Surgery or Steroid Epidural Injections
A steroid epidural is an injection that places steroid medication around irritated or inflamed nerves in the spine. While they do help patients avoid surgery, epidurals use very high-dose steroids that can cause severe side effects and actually reduce the body’s ability to heal.
Regenexx offers a variety of minimally invasive procedures that deliver ultra-precise spinal injections of platelet lysates (or in fewer cases, bone marrow concentrate) where needed, utilizing advanced imaging guidance to ensure precise placement into the injured area.
*DISCLAIMER: Like all medical procedures, Regenexx® Procedures have a success and failure rate. Patient reviews and testimonials on this site should not be interpreted as a statement on the effectiveness of our treatments for anyone else.
Platelet Treatments for Pain from Bulging or Herniated Discs
A bulging disc is also called a disc protrusion or bulge. This means that the outer covering of the disc (annulus) is partially torn or damaged and the inner gel is causing the area to bulge. This can put pressure on a spinal nerve and cause numbness and tingling (sciatica).
A herniated disc is also called a disc extrusion, slipped disc, sequestration, or “HNP” (Herniated Nucleus Pulposis). This means that the outer covering of the disc (annulus) is completely torn or damaged and the inner gel squirts out. This can put pressure on a spinal nerve or cause severe swelling and lead to numbness and tingling (sciatica).
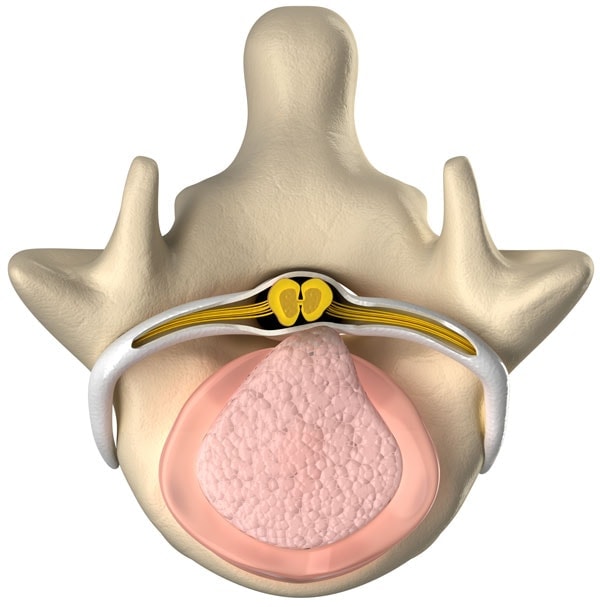
Treating Bulging and Herniated Discs
Platelet Lysate is often used in the treatment of Bulging and Herniated Discs. This very specialized Regenexx-developed procedure utilizes natural growth factors from the patient’s own blood platelets. Regenexx’s extensive experience in Platelet Lysate, Platelet-Rich Plasma, and Bone marrow Concentrate from the patient’s own body enables us to determine the best treatment options to address your source of pain.
Platelet Lysate Spinal procedures are administered with precise imaging guidance to target the specific areas needing treatment and may offer relief from lower back or neck pain, buttock, and leg pain, or numbness and tingling in the arms, hands, legs, or feet. It’s a highly specific, precise image-guided non-surgical treatment alternative for patients suffering from bulging discs and herniated cervical, thoracic, or lumbar disc-related problems, performed only by specially trained Regenexx Physicians.
A Better Option than Steroid Epidurals
A steroid epidural is an injection that places steroid medication around irritated or inflamed nerves in the spine. While they may help patients avoid surgery and can provide pain relief temporarily, epidurals use very high-dose steroids which can reduce the body’s ability to heal and can lead to severe side effects.
Regenexx Platelet Lysate is a very specific, precise image-guided injection-based alternative to a steroid epidural injection. It uses natural growth factors from the patient’s own body, derived from their own blood platelets, helping patients avoid surgery and the negative side effects of steroids.
Using Your Body’s Own Healing Agents for Degenerated Disc Pain: Bone Marrow Concentrate and Platelets
Because Regenexx was the first to develop this type of treatment modality, we have the experience and the broad spectrum of procedures that allow for the treatment of all of these conditions. Regenexx procedures provide highly specific, precise image-guided, non-surgical treatment options using the healing agents from your own body for patients suffering from the complications associated with degenerative disc disease. Our highly skilled Physicians carefully target the right procedure to the impacted areas of the spine using precise imaging guidance, so that patients may avoid spinal fusion surgery or frequent high-dose steroid epidural injections and their associated side effects.
Advanced Treatments for Degenerative Discs
Degenerated disc patients tend to lose disc height which can lead to a wide range of complications.
- Compressed nerves (stenosis)
- Facet joint overload leading to arthritis
- Lax ligaments that result in overall spinal instability
Our advanced Interventional Orthobiologic treatment protocol focuses on Platelet and/or Bone Marrow Concentrate from the patient’s own body deployed to treat disc movement due to lax ligaments and arthritic facet joints.
Each of these critical areas above may benefit from different types of procedures.
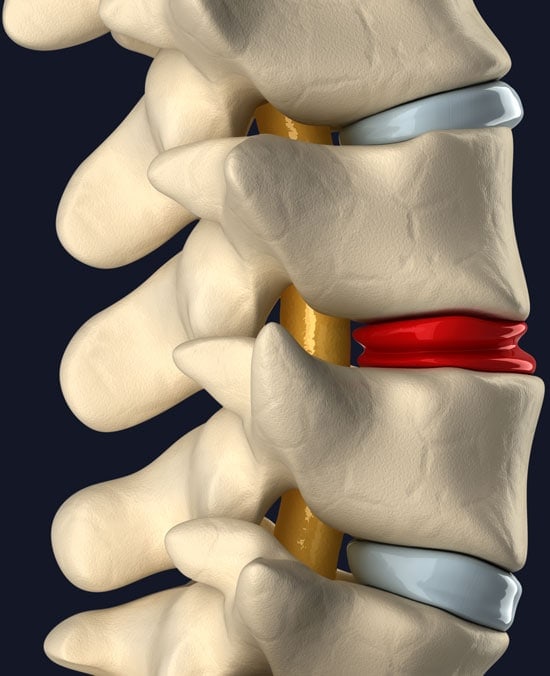
Advanced Treatments for Torn & Painful Discs
Disc tears are also called annular tears or HIZs (High-Intensity Zones) on MRI images. A patient with a painful and torn disc has “discogenic pain”. The outer covering of the disc can be torn due to injury and painful nerves can grow into the area, leading to low back pain, usually with sitting or activity. In addition, the tear in the disc may lead to noxious chemicals escaping and irritating the spinal nerve, which can lead to sciatica.
Patients with this type of disc damage and pain may benefit from a Regenexx Bone Marrow Concentrate injection procedure.
This highly specialized precise image-guided non-surgical procedure uses cells isolated from the patient’s own bone marrow. The bone marrow is collected using a special needle and advanced imaging guidance during an in-office procedure with your Regenexx Physician. The harvesting procedure is well tolerated by patients and many patients report experiencing no pain. After collection, the Bone Marrow is centrifuged to concentrate the healing cells, and unneeded cells are removed. These cells, along with a preparation of concentrated blood platelets, are injected the same day into the damaged disc, using precise advanced imaging guidance.
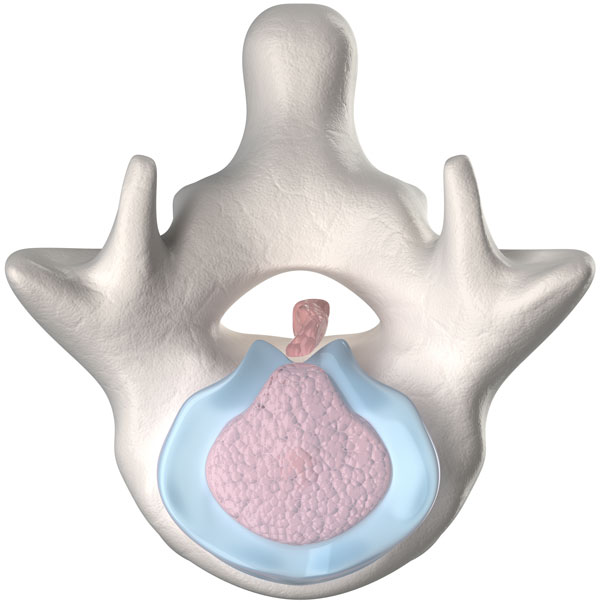
How Regenexx Procedures Work
Regenexx-SD is Bone Marrow Concentrate. These repair cells from your own body live inside all of us in various tissues, poised to leap into action to repair damage as it occurs. As we age or have big injuries, we may not be able to recruit enough of these cells to the site to fully repair the area. The Regenexx-SD Procedure helps overcome this problem by harvesting Bone Marrow from an area of the back of the hip that contains a dense population of these important cells and then concentrating those cells before precisely injecting them into the injured area using advanced imaging guidance. The goal of the procedure is to reduce pain and improve function by promoting the body’s own ability to heal naturally. This Patented Bone Marrow Concentrate Protocol can be used for a wide range of orthopedic conditions. Your Regenexx doctor will evaluate your condition and your imaging to determine whether a bone marrow concentrate or platelet-based treatment is the best option for your orthopedic condition.
Platelet Rich Plasma (PRP) and Platelet Lysate are Platelet procedures that contain healing growth factors from your own blood that promote your body’s natural ability to repair itself. The use of PRP to treat joint, tendon, ligament, and muscle injuries is becoming well known, thanks to exposure from professional athletes. Platelet injections have a stimulating effect on the repair cells within the targeted area, making those cells work harder to perform their natural job of healing the body. Like all Regenexx procedures, Regenexx SCP procedures are performed with high-level imaging guidance to ensure the most accurate placements of cells into the desired area. Our Advanced Platelet Procedures are more concentrated and purer than PRP created by the automated machines used at most regenerative medicine clinics, increasing its ability to stimulate the body’s natural healing response. Platelet procedures are commonly used for soft tissue injuries, mild arthritis, spine conditions, and around nerves.
Regenexx® Patient Success Stories
*DISCLAIMER: Like all medical procedures, Regenexx® Procedures have a success and failure rate. Patient reviews and testimonials on this site should not be interpreted as a statement on the effectiveness of our treatments for anyone else.